Technical Deep Dive • Anatomy, Pathways & Functions
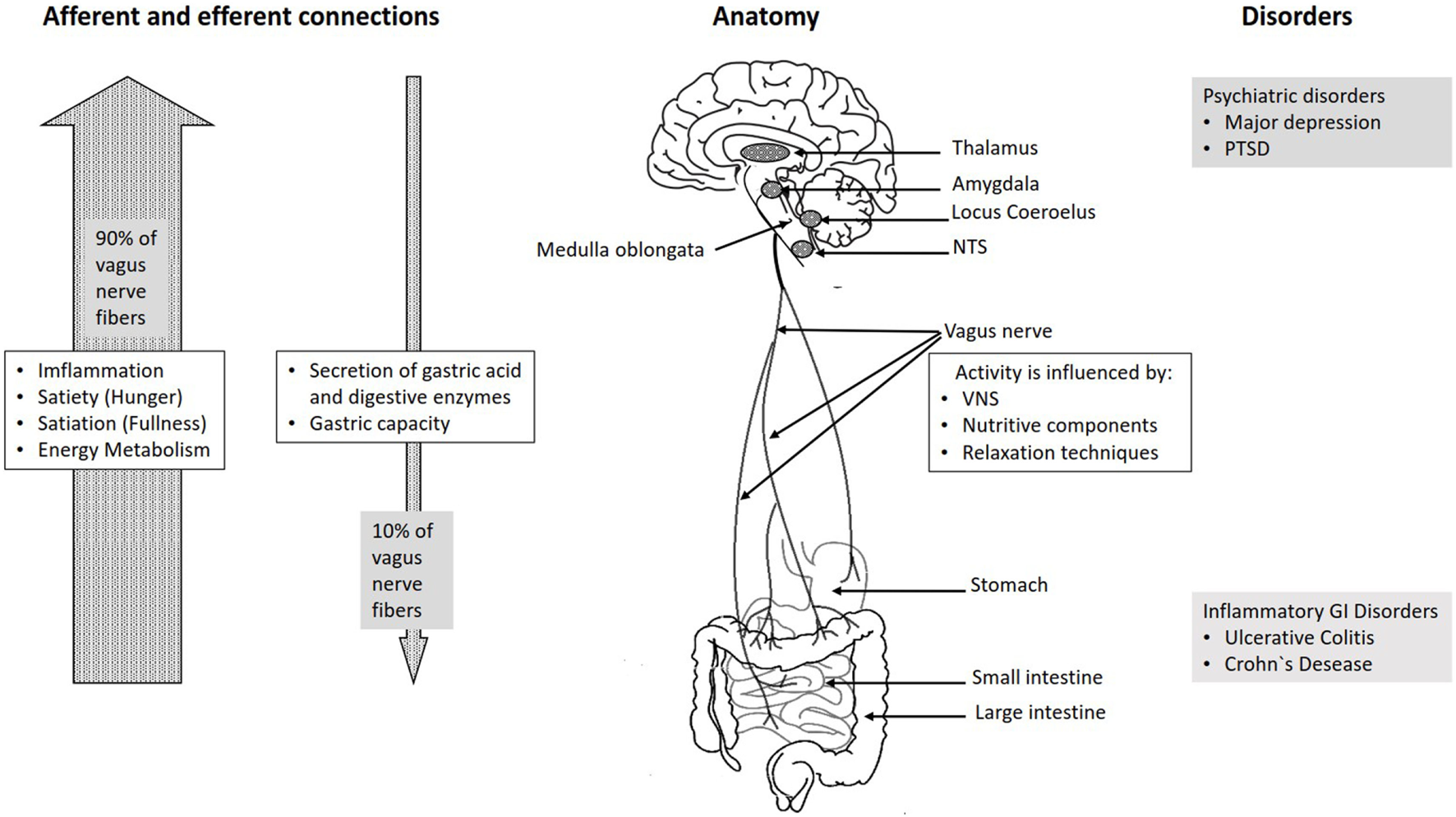
Afferent (sensory) and efferent (motor) connections of the vagus nerve (Frontiers in Psychiatry, 2018)
Origin and Full Course
The vagus nerve originates in the medulla oblongata of the brainstem, primarily from the dorsal motor nucleus (DMN – parasympathetic efferents), nucleus ambiguus (NA – motor to larynx/pharynx), and nucleus tractus solitarius (NTS – 80-90% sensory afferents). It exits the skull through the jugular foramen, descends in the carotid sheath, gives branches in the neck, thorax (cardiac, pulmonary, oesophageal), and abdomen (gastric, hepatic, celiac, splenic). It terminates at the splenic flexure of the colon.
Organ-by-Organ Functions
Cholinergic Anti-Inflammatory Pathway (CAP) – Detailed Mechanism
Vagus activation releases acetylcholine at the celiac ganglia. This activates the splenic nerve, which releases norepinephrine in the spleen. Norepinephrine binds β2-adrenergic receptors on ChAT-positive T-cells, which then release acetylcholine. Acetylcholine binds α7 nicotinic receptors on splenic macrophages, inhibiting NF-κB and STAT3 signalling and rapidly suppressing TNF-α, IL-6 and IL-1β production. This is the body’s primary neural brake on systemic inflammation.
Polyvagal Theory & Clinical Correlations
Low ventral vagal tone shifts the autonomic nervous system into chronic sympathetic dominance or dorsal shutdown, underlying treatment-resistant depression, anxiety, MCAS flares, long-COVID sensory hypersensitivities, central sensitization, and poorer cancer survival outcomes.